Dr. Manasi Thakur | Gynaecologist In Nagpur | Pregnancy, Delivery | Abortion | Cosmetic Gynecology
What is a Threatened Miscarriage?
Causes of Threatened Miscarriage
The exact cause is often unclear, but some common factors include:
Chromosomal abnormalities in the fetus (most common in the first trimester)
Chronic maternal conditions such as diabetes, lupus, high blood pressure, or thyroid disorders
Inadequate hormone production
Acute infections
Uterine abnormalities – fibroids, cervical weakness, abnormal placental growth, or carrying multiples (twins, triplets, etc.)
Lifestyle factors – excessive caffeine, alcohol, tobacco, or cocaine use
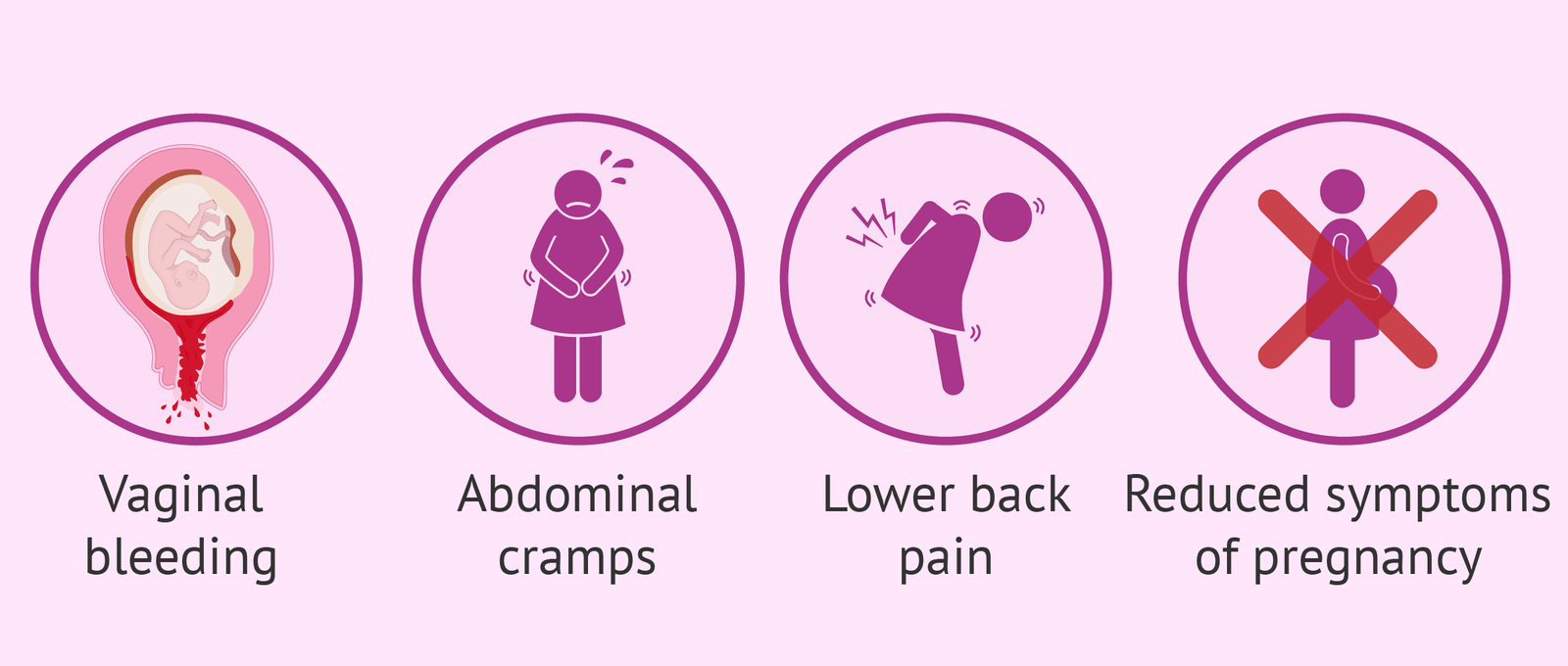
Signs of Threatened Miscarriage
The symptoms are usually mild, but any pregnant woman experiencing them should seek immediate medical care at Zenith Hospital, Nagpur, under Dr. Manasi Thakur:
Vaginal bleeding – usually light, brownish, or bright red. Sometimes heavy, especially in later pregnancy.
Bleeding is often painless, but may be associated with backache or lower abdominal pain.
Pain often appears when bleeding starts.
Diagnosis of Threatened Miscarriage at Zenith Hospital, Nagpur
Dr. Manasi Thakur performs a detailed medical, surgical, and obstetric history along with a careful clinical examination to identify possible causes.
Investigations include:
Blood tests: Hemoglobin, hematocrit, ABO and Rh grouping. Blood transfusion may be required if miscarriage becomes inevitable, and anti-D gamma globulin is given to Rh-negative, non-immunized women.
Serum progesterone: A value of 25 ng/mL or more generally indicates a viable pregnancy in about 95% of cases.
Serial serum hCG levels: Helpful in assessing fetal well-being.
Ultrasonography: To evaluate fetal heartbeat, growth, and viability.
Management of Threatened Miscarriage
Rest: Bed rest for a few days until bleeding stops. Prolonged inactivity is not advised.
Pain relief: Diazepam 5 mg twice daily may be prescribed.
Hormonal support: Progesterone therapy has shown positive outcomes in some cases.
Prognosis of Threatened Miscarriage
In about two-thirds of cases, the pregnancy continues beyond 28 weeks.
In the remaining cases, miscarriage occurs.
Even if pregnancy continues, there may be a higher risk of complications such as:
Preterm labor
Placenta previa
Intrauterine growth restriction (IUGR)
Fetal anomalies
